Organization
National Kidney and Transplant Institute
Best Practice Focus Area/s
Leadership, Citizens / Customers, Operations
Year Implemented
March 2020
This is a GBPR entry
Summary
As the COVID Crisis Management Team was mobilized, human resource concerns, alternative work arrangements, transportation, accommodation, logistics, supply management, procurement, etc., were also addressed. Medical and surgical practices were recalibrated in such a way that the activities were suspended at the outpatient department and limited admissions to only urgent and emergency renal cases. Subsequently, “telehealth†was employed, and surgical cases resumed. Control and containment of the transmission of the disease were paramount because it is the essence of protecting immunocompromised patients. The hospital specializes in renal diseases, not pneumonia which should be the domain of the lung specialty center, but then there were renal cases who developed pneumonia, and there were severe septic pneumonia cases who went into renal failure and needed hemodialysis and even hemoperfusion. When patients come to the hospital, the first course of action is to accommodate them and take care of them the best way.
Background and Problem
Part of controlling the spread of the disease is to protect the healthcare workers and the patients of the NKTI. Another is to contain the disease and not let it spread. However, there were not enough beds and space under the roof. When there were no COVID RT-PCR tests, the hospital relied more on a high index of suspicion. Unless proven otherwise, a patient with pulmonary symptoms was tagged as a “COVID†patient at the triage. Some waited in their cars. They sit side by side in wheelchairs and lie very near each other on the stretchers without physical distancing. Others cannot be attended to immediately when incoming moribund patients must be intubated. There was no vacancy in the intensive care unit (ICU). Watchers also conglomerate and, later, become infected. Likewise, healthcare workers (HCWs) also become infected.
During the early months, COVID referral centers were also congested and not well-equipped. Networking was not effective. The gate for cars going to the Emergency Room (ER) had to be closed as patients also occupied the supposed drop-off areas near Gate 2. Whether on dialysis or not, renal and non-renal patients just kept on coming to the hospital. Patients should be cohorted before admission to a regular room. It was impossible to cohort them until the COVID swab tests and chest x-ray was administered and the results were released. “Congestion†can look like pneumonia when patients are under-dialyzed or have missed dialysis due to a lack of transportation during lockdowns.
The hospital’s total bed capacity is 381, but it only has an implementing bed of 302 because of the conversions made to some patient rooms to donning and doffing areas and observance of physical distancing. The ER has only 30 beds, with an extension of 14 beds. With patients under investigation (PUI), patients under monitoring (PUM) averaging, and COVID positives with a running average of 130-140 a day, they had to find a way to put a roof on the field. The ER occupies an area of almost 250 square meters. In the vicinity of the ER is a covered tunnel that separates it from a commercial bank. Across the bank is the parking lot. These areas would soon be commandeered to become the “Tent Field.†Renal patients on dialysis are urgent and emergency cases who need insertion/creation of vascular access and “troubleshooting†of their clogged vascular access. They too had to be screened before any surgery. All patients should undergo COVID testing and chest x-ray. They cannot be done in a room, which is also being used by non-COVID patients, as cross-infection should be prevented.
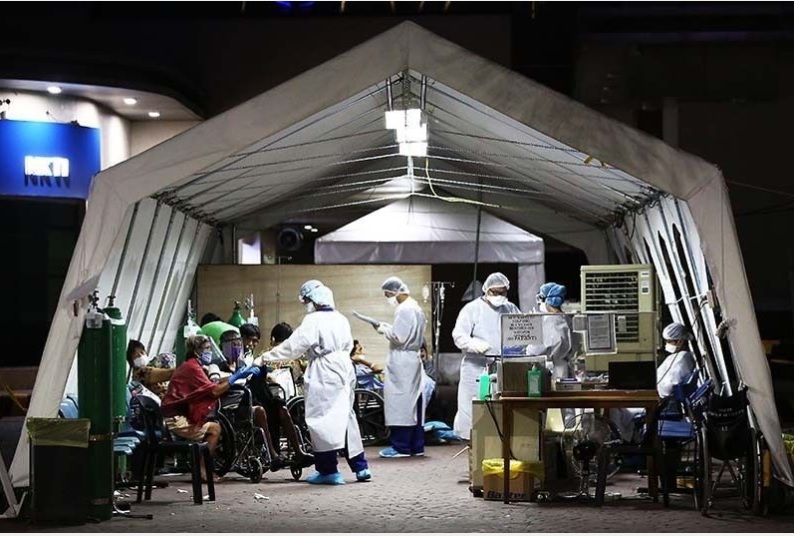
Solution and Impact
In front of the ER, from a mere triage, the “manger†expanded and built tents of different colors, sizes and heights. Most of these are donations. These resources were carefully managed to serve their purpose. Some donations were tents, electric fans, air-conditioner units, cot beds cushions, ventilators, and medical and surgical supplies. They built a “Tent Field Hospital†for COVID and retrofitted “Hotzones,†harnessing the art and science of engineering, the highlights of which included the provision for laminar airflow, negative pressure, elevated floorings, air-conditioning, installation of exhausts, electrical and water sewer lines, local area network, and oxygen supply. The number of tents increased, rapidly occupying the tunnel, the parking lot, towards Gate 2, and almost encroaching East Avenue. There were tents for cohorting patients, pediatric patients, a makeshift ICU, hemodialysis and peritoneal dialysis stations, watchers, a radiology tent with an ultrasound and x-ray machine, and a satellite operating room. As part of the emergency response, the Eden field (formerly occupied by an illegal establishment), a modular COVID hemodialysis facility was built.
The second floor of the main hospital was retrofitted to modify air exchanges in preparation for more admitting patients. Four wings compose the main building: Units 2A, 2B, 2C, and 2D, the 2B and the 2C extensions – comprising the 80-bed hot zone. In these areas, acrylic curtains were installed. 2A was occupied by patients with negative (-) RT-PCR but with pneumonia, suspicious of COVID. 2B to 2D were occupied by positive (+) RT-PCR patients with increasing severity of pneumonia. 2C was dedicated to isolation rooms for HCW, and 2B extension became a 4-station COVID dialysis room. In-patient dialysis stations were converted to outpatient COVID patients who free-standing dialysis centers refused. Four beds at the ICU were dedicated to critical COVID cases. During a COVID surge, the Gymnasium had to be converted into a COVID ward consisting of 30 beds with strict observance of the required distancing.
Because of this extraordinary measure, more patients were managed optimally, physically, and medically. Even during the second surge, NKTI was well-armed. The COVID Manual, with its guidelines, underwent a second edition. The NKTI “Contingency Plan for COVID Surge†was crafted and will apply to any infectious disease.
Milestones
The NKTI management started creating the COVID Crisis Management Team and simultaneously modified the physical set-up of the hospital as early as March 2020. Controls were provided as regards the ingress and egress of persons in the hospital. Ancillary support services include free accommodation, meals, and transportation to healthcare workers. The main thrust of the NKTI management is to be resilient and not to suspend hospital operations since most NKTI patients are chronic and require lifetime treatment, e.g., patients under dialysis. A COVID RT-PCR was also built, eventually accredited by the DOH. A modular COVID HD was also built alongside facility conversions, such as patient units and the gymnasium.
